Colorectal cancer (CRC) is one of the most common types of cancer diagnosed in the UK. About 41,000 people get cancer in the large bowel each year in the UK. In 2020, the WHO reported that colorectal cancer accounted for 10% of the cancers diagnosed annually. (Global Cancer Observatory)
This article will bring to your attention data on indications and outcomes of SABR on patients with CRC, and discuss MVision’s guideline-based solution for your radiotherapy workflow.

SABR for Colorectal Cancer
Stereotactic ablative radiotherapy (SABR) is a highly focused form of radiation treatment that administers an intense dose of radiation concentrated to a tumour, while limiting the radiation to the surrounding organs. According to the NCCN guidelines, SABR can be considered for patients:
- With a limited number of metastases and when surgical operations are not possible
- With recurrent cancer in a previously irradiated region (Benson AB, et. al.)
A 2019 systematic review and meta-analysis of SABR for CRC pulmonary metastases included data from 18 observational studies. There were variations in the treatment schedules and other therapies between the set of studies. However, the collected information on the outcomes is promising. The local control of 686 colorectal pulmonary metastases was 81% after one year and 60% after three years. The review found the overall survival rate after three years was 52% in the subgroup of patients whose combined total of lung metastases was 567. No mortality was associated with the procedures, and the grade 3 toxicity (severe and undesirable toxicity) was below 3% when observed. (Cao, Christopher, et. al.)
SABR for CRC liver metastases was analyzed in a systematic review of the results published in 18 studies encompassing 656 patients. The local control was 67% at one year and 59.3% at two years. The overall survival at two years was 56.5%, and severe liver toxicity was 8.7%. (Petrelli, F., et. al.)
A single-center retrospective study from the Netherlands reported data on outcomes of 90 patients with liver metastases (77% of the 97 metastases had CRC as origin). The study concluded that a higher dose of SABR was more efficient. The local control rate at two years was 90% for the high dose group and only 60% for the lower dose group without increasing toxicity. There was a correlation between the tumor volumes created with the local control and the overall survival excluding dose.(Kok, Esther, et. al.)
A China-based published interesting results. The team treated 94 CRC patients who had a combined total of 162 metastases (mostly in the lung, liver, brain, or lymph nodes). All patients treated previously underwent radical surgery, with a majority having less than five synchronous or growing metastases.
The best results were seen among patients who had synchronous metastases. Their median interval of no disease progression was 12.6 months. One year after SABR, more than 1/3 of patients did not need to start or change the systemic therapy. This positive effect was obtained also after the second use of SABR, suggesting that subsequent “lines” of repeated SABR have cumulative benefits for patients to delay further progression. Another interesting finding was that SABR postponed progression from the oligometastatic to the polimetastatic state. The median time to this progression was 20.8 months. Patients who became polimetastatic were significantly worse: with a 69.3% over survival rate at two years compared to 94.1% of those who remained oligometastatic. All the patients who experienced pain before SABR had a decrease of this symptom, subsequently improving their quality of life.
The authors also proposed a nomogram for predicting the outcomes of such cases, taking into account the independent factors for survival, which they identified on multivariate analysis – the indication, the performance status, pre-SABR CEA value, and PTV volume. (Ji, Xiaoqin, et. al.)
Results of reirradiation of rectal cancer local recurrence was reported by a team from UK. Researchers used SABR for inoperable patients with small-volume pelvic relapse and achieved a local control of 69% at two years. They observed Grade 3 toxicity in only one of the patients and reported no grade 2 toxicity. (Smith, T., et. al.)
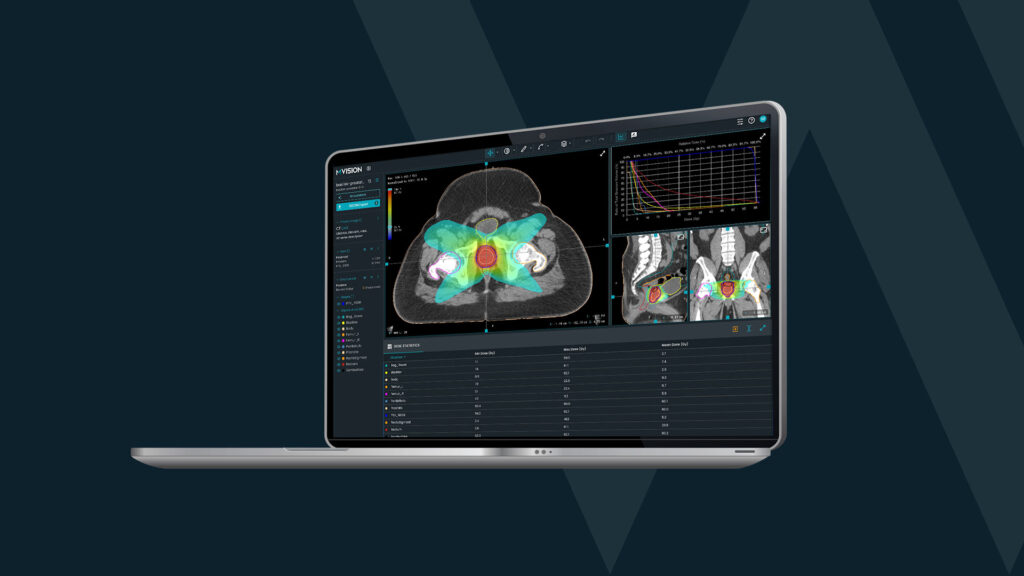
Guideline-Based Segmentation, GBS™, for your CRC Workflow
MVision’s Abdomen & Thorax Model follows consensus guidelines, including RTOG, for consistency and quality treatment planning.

MVision’s GBAIS™ SaaS Solution
MVision AI is the pioneer of guideline-based AI segmentation, GBAIS™, radiotherapy software. Our deep learning system helps you automate organ-at-risk contouring, in addition to lymph node regions, for streamlined cancer treatment planning. Our software complies with HIPAA, and GDPR, bringing the highest quality radiotherapy planning SaaS solution for your oncology department.
Book a demo to explore GBAIS™ for your clinic.
MVision AI is active on LinkedIn, Twitter, Facebook, and Instagram. Follow us on social media to stay up-to-date on the latest MVision AI news.
Are you eager to learn more? We welcome you to contact MVision AI:
c/o Terkko Health Hub, Haartmaninkatu 4, 00290 Helsinki, Finland.
Tel: +358 (0) 40 5489 229
Email: info@mvision.ai
For media inquiries:
+358 40 500 7915; pr@mvision.ai
Sources
Benson AB, et. al. “Colon Cancer, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology.” Journal of the National Comprehensive Cancer Network : JNCCN, U.S. National Library of Medicine, https://pubmed.ncbi.nlm.nih.gov/33724754/.
“Cancer Today.” Global Cancer Observatory, https://gco.iarc.fr/today/data/factsheets/cancers/10_8_9-Colorectum-fact-sheet.pdf.
Cao, Christopher, et al. “A Systematic Review and Meta-Analysis of Stereotactic Body Radiation Therapy for Colorectal Pulmonary Metastases.” Journal of Thoracic Disease, AME Publishing Company, Dec. 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6988072/.
Ji, Xiaoqin, et al. “Outcomes of Stereotactic Body Radiotherapy for Metastatic Colorectal Cancer with Oligometastases, Oligoprogression, or Local Control of Dominant Tumors.” Frontiers, Frontiers, 1 Jan. 1AD, https://www.frontiersin.org/articles/10.3389/fonc.2020.595781/full#f3.
Kok, Esther N.D., et al. “High versus Low Dose Stereotactic Body Radiation Therapy for Hepatic Metastases.” Clinical and Translational Radiation Oncology, Elsevier, 27 Nov. 2019, https://www.sciencedirect.com/science/article/pii/S2405630819301119.
Petrelli F, et. al., “Stereotactic Body Radiotherapy for Colorectal Cancer Liver Metastases: A Systematic Review.” Radiotherapy and Oncology : Journal of the European Society for Therapeutic Radiology and Oncology, U.S. National Library of Medicine, https://pubmed.ncbi.nlm.nih.gov/29997034/.
Smith T; et. al; “Stereotactic Body Radiation Therapy Reirradiation for Locally Recurrent Rectal Cancer: Outcomes and Toxicity.” Advances in Radiation Oncology, U.S. National Library of Medicine, https://pubmed.ncbi.nlm.nih.gov/33305093/.